Search
The extent of lung hypoplasia impacts the survival and severity of morbidities associated with congenital diaphragmatic hernia.
Jane Pillow BMedSci (Dist) MBBS, PhD (Dist) FRACP Head, Developmental Chronobiology jane.pillow@thekids.org.au Head, Developmental Chronobiology
Understand how bronchopulmonary dysplasia (BPD) and antenatal and postnatal factors influence diaphragmatic functional effectiveness in very preterm infants.
Surfactant is a well-established therapy for preterm neonates affected by respiratory distress syndrome (RDS). The goals of different methods of surfactant administration are to reduce the duration of mechanical ventilation and the severity of bronchopulmonary dysplasia (BPD); however, the optimal administration method remains unknown.
Preterm infants are often vitamin A deficient, and vitamin A has functions that could mitigate the processes that lead to bronchopulmonary dysplasia. Therefore, supplementation of preterm infants with vitamin A to reduce the risk of bronchopulmonary dysplasia makes inherent sense.
Lung inflammation and impaired alveolarization precede bronchopulmonary dysplasia (BPD). Glucocorticoids are anti-inflammatory and reduce ventilator requirements in preterm infants. However, high-dose glucocorticoids inhibit alveolarization. The effect of glucocorticoids on lung function and structure in preterm newborns exposed to antenatal inflammation is unknown. We hypothesise that postnatal low-dose dexamethasone reduces ventilator requirements, prevents inflammation and BPD-like lung pathology, following antenatal inflammation.
Perinatal inflammation increases the risk for bronchopulmonary dysplasia in preterm neonates, but the underlying pathophysiological mechanisms remain largely unknown. Given their anti-inflammatory and regenerative capacity, multipotent adult progenitor cells (MAPC) are a promising cell-based therapy to prevent and/or treat the negative pulmonary consequences of perinatal inflammation in the preterm neonate.
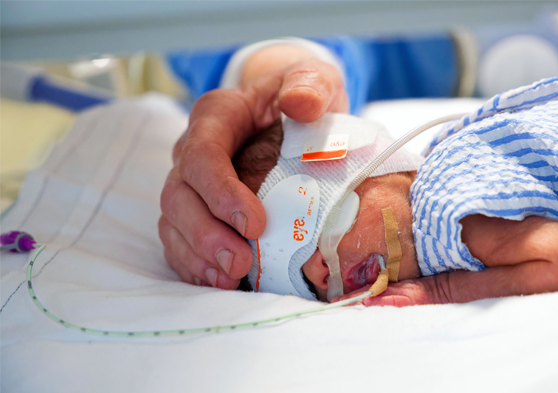
The CIRCA DIEM Study is a clinical research study being coordinated by the Chronobiology Team at The Kids Research Institute Australia, who are based in Perth, Western Australia and involving research teams from around the world.
A previous systematic review showed that intramuscular vitamin A supplementation reduced the risk of bronchopulmonary dysplasia (BPD) in very-low-birth-weight (VLBW) infants. However, more recent studies have questioned this finding.
Vitamin A has anti-inflammatory and immune-modulating properties. We aimed to assess whether enteral water-soluble vitamin A supplementation in extremely preterm infants decreases fecal calprotectin, a marker of intestinal inflammation.
