Search

Institute Director; Head, Strep A Translation; Co-Founder of REACH
As Head of Aboriginal Research Development at Telethon Kids, Glenn Pearson believes his work brings us closer to identifying the real and whole Australian story
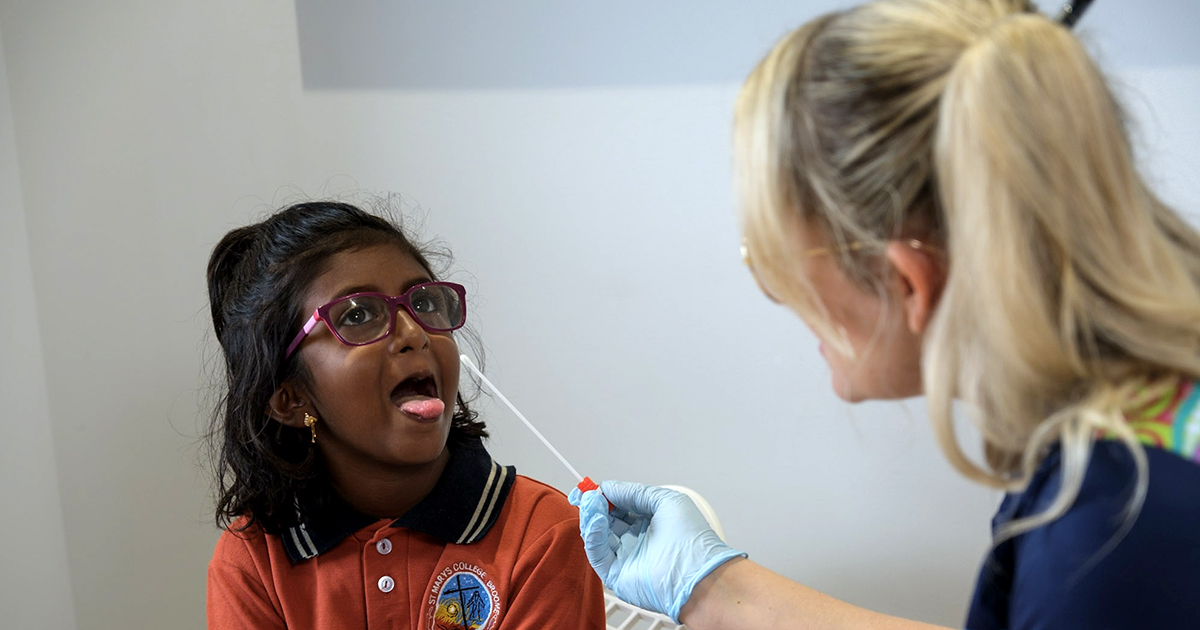
New research has revealed that molecular point-of-care testing (POCT) can significantly improve detection of Group A Streptococcal (Strep A) pharyngitis compared to laboratory culture – particularly in remote communities, where results can take up to seven days – unlocking a major opportunity to prevent rheumatic

A team led by Dr Joseph Kado from the Wesfarmers Centre of Vaccines and Infectious Diseases, based at The Kids Research Institute Australia, and The University of Western Australia (UWA) has been awarded $5 million by the Federal Government in a major push to prevent rheumatic heart disease across the Pacific.

Instant diagnosis and treatment of potentially life-threatening Strep A infections is now very close to reality across Australia’s remote and regional areas thanks to molecular point-of-care testing (POCT) that slashes result times from five days to just minutes.

There are calls for a significant and urgent injection of $40 million in funding to tackle Rheumatic Heart Disease (RHD) following Monday night’s Four Corners episode.

Children at risk of potentially life-threatening Strep A infections no longer have to wait five days for timely treatment, thanks to a The Kids Research Institute Australia study conducted in the remote Kimberley region of Western Australia.

When Katrina took her daughter Tenaya to the local emergency department for the fourth time, she was determined she wouldn’t be leaving without answers.

It's been a huge year for those working to eliminate rheumatic heart disease (RHD), with breakthroughs including $35M in funding to develop a Strep A vaccine.

End RHD CRE News & Events
